
Genetics mean that Asian populations are more likely to store fat as dangerous internal fat wrapped around their organs. People with problematic amounts of this internal fat may still look quite slender, but develop serious obesity-related health issues.
© Getty Images/xPACIFICA
For a variety of genetic reasons, obesity in Asia isn’t always as obvious as in the West, but it is a major problem — complicated by the fact that Asian studies come back with very different metabolic responses.
“The obesity you see in Asia is internal, it’s visceral. You may look skinny and have a pretty impressive BMI, but also suffer from an insidious metabolic condition,” explains Christiani Jeyakumar Henry, director of Clinical Nutritional Sciences at A*STAR’s Singapore Institute of Clinical Sciences (SICS)1.
As a result, Asian people who don’t fit the typical expectations of what obesity looks like may still be described by its formal definition — fat accumulation that has an effect on health, such as causing diabetes.
Asian metabolisms: internal body fat, higher blood sugar
“The diabetes rate in Asians is very high for example, even among those who have the same body weight as Caucasians,” says Shigeki Sugii from A*STAR’s Singapore Bioimaging Consortium (SBIC). The greater percentage of people with fat wrapped around internal organs, known as visceral fat, is probably why Asians have a higher prevalence of metabolic and obesity causing diseases.
The most recent data from the International Diabetes Federation indicates that in 2015, 415 million people had diabetes, more than half of whom lived in Asia. “If you have an HbA1C of say seven in Europe and you talk to a doctor,” says Henry, “they say, ‘Well that’s pretty good, well done’.” But he says, in Asia people with seven and eight “are ending up with [diabetes-related] renal failure”.
About six years ago Henry moved from Oxford in the United Kingdom to set up a center studying metabolism in Singapore, the perfect place to launch studies specific to Asian ethnicities. Singapore is the world’s most densely populated city and home to large cohorts of Malay, Chinese and Indian residents — which means that Henry’s scientists at the SICS Centre for Clinical Nutritional Sciences are leaders in the study of Asian metabolic responses.
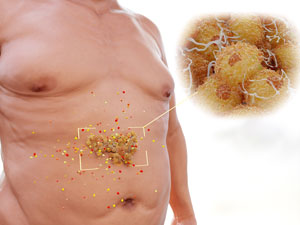
As well as a tendency towards storing fat as internal visceral fat (pictured above), people of Asian descent typically have a higher blood sugar response to carbohydrates than Caucasians, meaning that diets rich in rice may be causing an increasing obesity problem across Asia.
© Getty Images/selvanegra
Asian groups across the board — whether Malay, Indian or Chinese — says Henry, all have a significantly higher glycaemic response to carbohydrates than western groups2. Glycemic responses are the effect a meal has on your blood sugar and insulin levels, which can increase your fat accumulation from carbohydrates and heighten the risk of developing diabetes, one of the most serious consequences of obesity. “So you can’t use the normal BMI cut-off to articulate [an Asian person’s] risk of getting Type II diabetes,” says Henry.
Diabetes dramatically increases the risk of cardiovascular problems, nerve damage (neuropathy) and kidney damage (nephropathy), among other things — all expensive burdens on healthcare systems. Henry says increasing knowledge about Asian metabolic responses will change what foods governments advocate for Asian populations. High carbohydrate diets send Asian insulin levels “through the roof” says Henry. Rice, in particular, is a problem. “In Asia people are eating up to 700 grams of cooked rice in a day, sometimes at breakfast, lunch and supper… We need to spend many more resources and much more money on looking at food competence, as we have done with pharma, because how on earth are we going to manage up to 50 million people who have Type II diabetes in China alone?”
The classical nutrition paradigms say we should eat less fat and therefore more carbohydrate, Henry adds. “That may be the worst thing for us to advise Asians because high carbohydrate, high glycemic index foods may be the reason why people in Asia, who are on a very low fat diet, are highly susceptible to Type II diabetes and obesity.”
The subtleties of smell, texture and taste
Tackling obesity often starts with looking at the foods you eat and how you eat them. Ciarán Forde is a principal investigator at the Clinical Nutrition Research Center (CNRC) where he and his team have been studying how Singaporean children eat, and how this relates to energy intake and body composition.

A team at the Clinical Nutrition Research Center at A*STAR describe what they call an ‘obesogenic eating’ style as an opportunity to intervene and change eating behaviours using a ‘food-based’ approach.
© Getty Images/Ryan Pyle
Their research, which was published earlier this year, highlights that children who eat with larger bites that are chewed less tend to consume more energy per meal, and have higher fat mass and body weight3,4. The team describe this ‘obesogenic eating’ style as an opportunity to intervene and change eating behaviors using what they call a ‘food-based’ approach.
“The sensory properties of foods can stimulate food-related behaviors and directly influence energy intake over time” says Forde. Food texture, for example, has a direct effect on bite size and chew rate and can influence the calories consumed during a meal through its effect on eating rate. Odors can also stimulate sensory-specific appetites and people receive signals on nutrient density from the taste, quality and intensity of their food.
His team looked into ways of using sensory experiences to influence calorie selection and intake, and have developed novel approaches to reducing calorie density and maintaining satisfaction using approaches like slowing eating rates with harder, more textured foods5, 6.
Good fats – white, brown and beige
But, tackling obesity could become even easier. Feng Xu, who works for the A*STAR Institute of Molecular and Cell Biology (IMCB), is another researcher who moved across the world, in this case from California, to work at A*STAR’s biomedical research hub. He’s focused on one of obesity’s hottest topics, brown and beige fat.
Unlike white fat, which is primarily designed to store energy, brown fat is a rarer type that burns energy for heat when a person is cold — a process known as thermogenesis. Once thought to be present only in babies, brown fats were re-discovered in adult humans in 2009 by improved PET-CT scan sensitivity. In the flurry of research since, it has been found that white fats can also be browned by an increase in their internal fat burning engines, mitochondria — making them more like brown fats. These have been dubbed beige fats.

Here, brown fat (left) with small fat vacuoles and more fat burning mitochondria (darker purple), is compared to white fat, with large fat vacuoles and less mitochondria. Until improved imaging found small amounts of fat-burning brown fats in adults in 2009, brown fat was thought only to exist in babies. A wave of research is now looking into how to increase or enhance brown fat to treat obesity
© vetpathologist/Shutterstock
Weight-loss medications have had a bad name since the detrimental effects of amphetamines — notably heart attacks — forced the US Food and Drug Administration to remove them from the US market in the 1960s. However, treatments that enhance brown fat could be akin to the magic bullets these claimed to be, as increased brown fat activity may improve our bodies’ capacity to burn fat. Recently, Xu used epigenomic profiling and bioinformatic analysis to search for novel regulators that promote brown fat’s energy expenditure7. In addition to the multiple protein factors identified in the study, he also discovered a micro-RNA, known as miR-32, that enhances brown fat activity. In a study published in Cell Reports in May, Xu and co-workers found that miR-32 is significantly induced in brown fat when exposed to the cold8. And, up-regulation of miR-32 leads to increased production and secretion of a circulating factor called FGF21 from brown fat, which further promotes white fat browning.
This study provides the first example of a brown fat microRNA that enhances subcutaneous white fat browning through a long-range effect, mediated by FGF21. In short, with a better understanding of this process, Xu thinks “there is a potential for miRNA-32 mimics to be explored for their function in promoting thermogenic activity in human brown fat to enhance the fat burning effect”.
Shigeki Sugii, group leader of the Fat Metabolism and Stem Cell Group at SBIC, also wants to promote brown fat’s effects and uses stem cells to study and target visceral fat – ‘bad fat’ that heightens metabolic problems. Earlier in his career he worked on small molecule drugs. “At that time I felt the limitations of small molecules in drugs, particularly for metabolic diseases, because diabetes is a chronic disease and you take the drugs for a long time,” says Sugii. Most drugs are made from small molecules, as their size lets them diffuse across cell membranes to affect bodily functions, but, cautions Sugii, these molecules often have side-effects.
Sugii instead wants to improve visceral fat function by inserting brown/beige fats made from stem cells into it — making it more like the fat just under the skin (better fat), which is known to have more beige fats9. To do this, he is currently working on improving the method of making stem cells into beige fat (and to image this process). The long-term goal is definitely to have people use stem cells to treat obesity. “It’s more effective and it can be more targeted,” he says.
Short- and long-term solutions

Images of two mice (middle) and their MRI cross sections (bottom) show reduced visceral and subcutaneous fat in the mouse treated with narciclasine, a natural compound extracted from wild daffodils.
Reproduced from Ref. 10 and licensed under CC-BY-4.0 (https://creativecommons.org/licenses/by/4.0/) © 2017 Sofi G. Julien et al.
In another recent study, Xu and his co-workers found that narciclasine, a natural compound purified from wild daffodils, has the potential to be developed into a novel anti-obesity drug. “Plant extracts containing this compound were used 2,000 years ago by Greek people treating tumors. From literature we knew that many cancer drugs changed the metabolism in cancer patients, so we thought that maybe narciclasine could also make a change in the metabolism,” says Xu.
In this study published in February, his team administered the drug to mice being fed excessive calories and found that the compound prevents the mice from becoming obese by increasing energy expenditure. Moreover, narciclasine promotes fat clearance from peripheral metabolic tissues, improves blood metabolic parameters, and protects these mice from the loss of voluntary physical activity. Further investigation suggested that narciclasine achieves these beneficial effects by promoting fatty acid consumption in the skeletal muscle10.
Henry points out that one of the most obvious issues with obesity research in Asia is that most of the studies to date come from the West, and do not focus on the Asian physique. This is coupled with the fact that increased living standards and consumption across the region have accelerated the occurrence of obesity.
However, there is plenty of work in the pipeline — Asia is a huge market says Henry, and many of the world’s top companies are already investing a lot of money in understanding and solving the region’s unique issues.
The A*STAR-affiliated researchers contributing to this research are from the Singapore Institute of Clinical Sciences (SICS), Clinical Nutrition Research Center (CNRC), Singapore Bioimaging Consortium (SBIC) and the Institute of Molecular Cell Biology (IMCB).




