Remember those childhood memories of diving face first into pillowy clouds of cotton candy? The spun sugar confection is made by spinning heated sugar in a rotating vessel, with the centrifugal force creating fine, interwoven threads of sweet goodness.
A biomedical engineering technique called wet electrospinning uses a similar concept. Jets of polymer solutions are extruded from a spinneret and deposited on a liquid bath that serves as a collector, forming three-dimensional, sponge-like matrices that mimic anatomical structures such as the dermal layer of the skin.
Jiah Shin Chin, a Research Fellow at the A*STAR Skin Research Labs (A*SRL), said that electrospun scaffolds offer hope to the millions worldwide living with chronic, non-healing wounds. Chin’s team has been devising different electrospinning techniques for next-generation skin scaffolds for use as chronic wound dressings.
“We wanted to create a topography that helps coax fibroblasts and endothelial cells to enter and populate the scaffold,” Chin said. “In that way, keratinocytes can cross over the scaffold to close the epidermal barrier and heal wounds.” The wet electrospun scaffolds would be a step up from conventional dressings and scaffolds which, despite their promise, cannot fully integrate with human skin and facilitate complete healing, Chin explained.
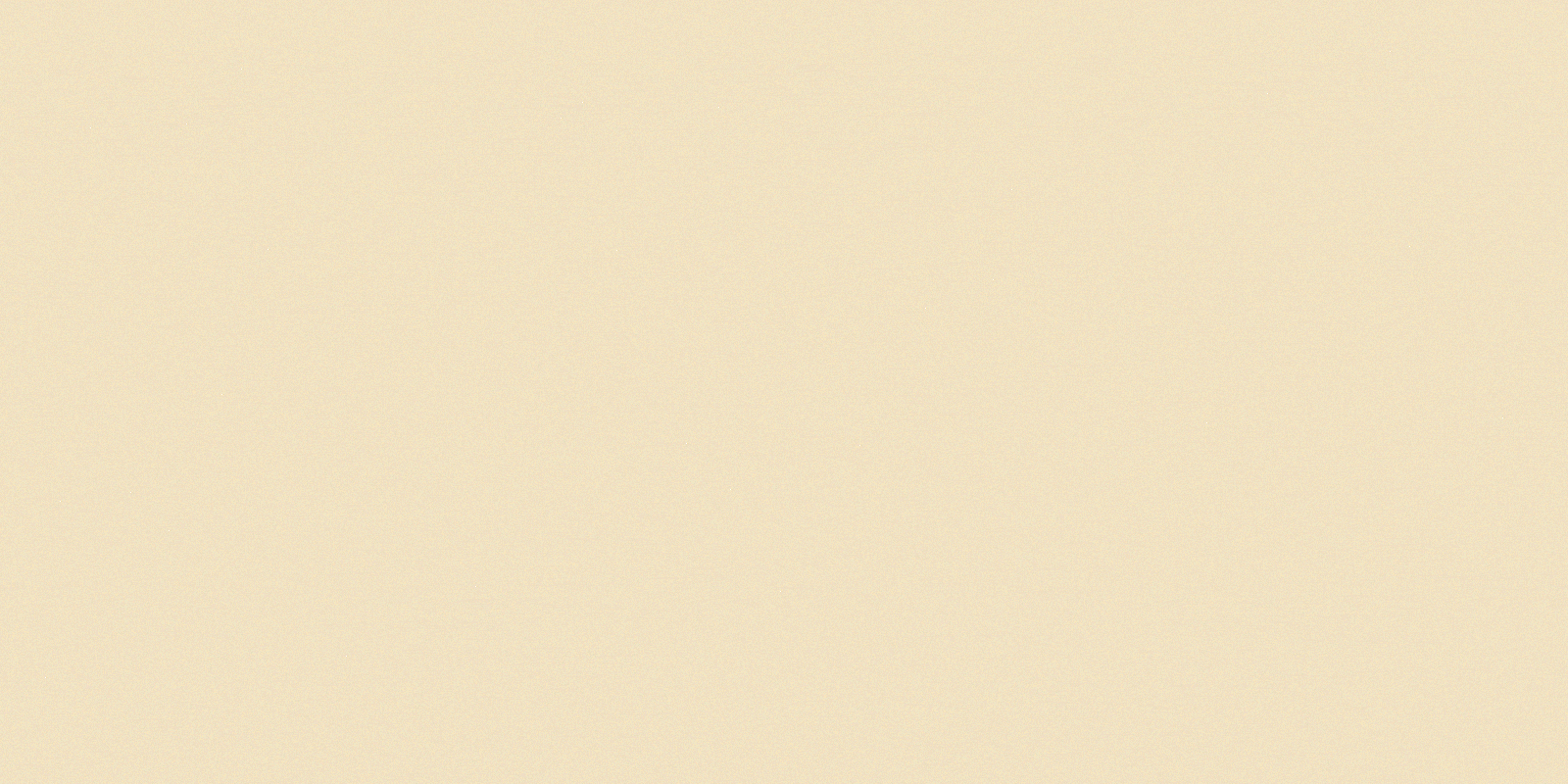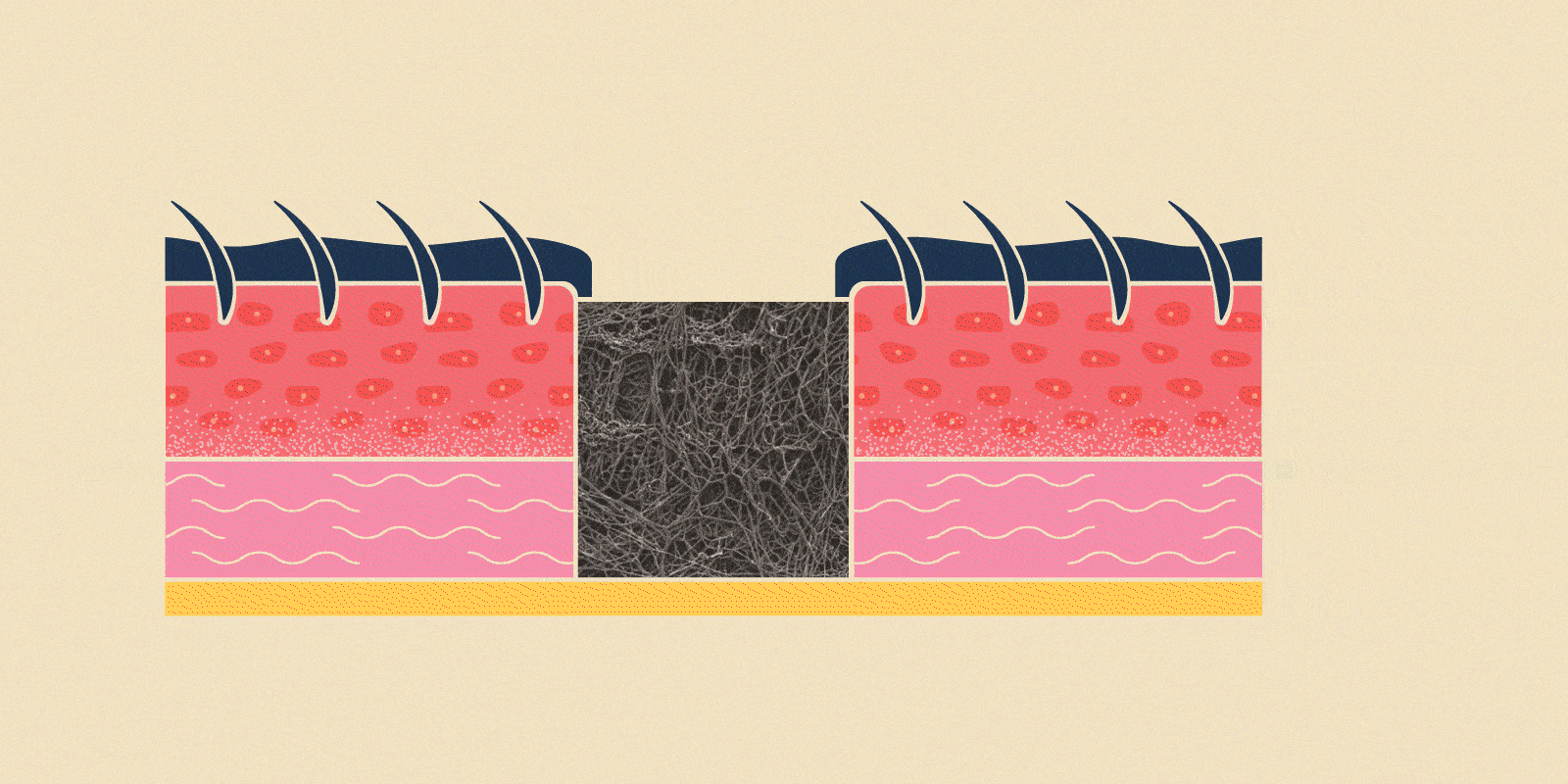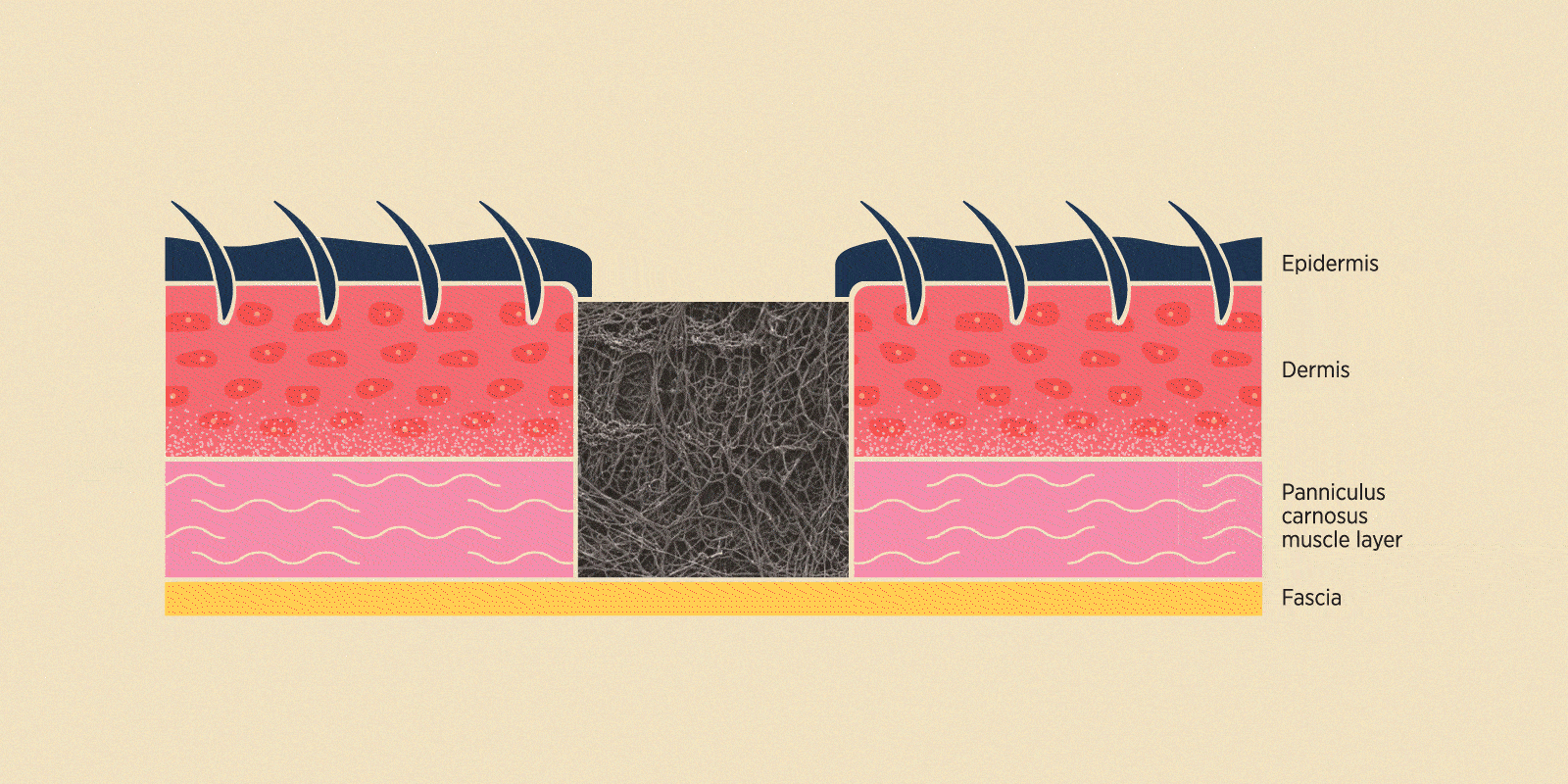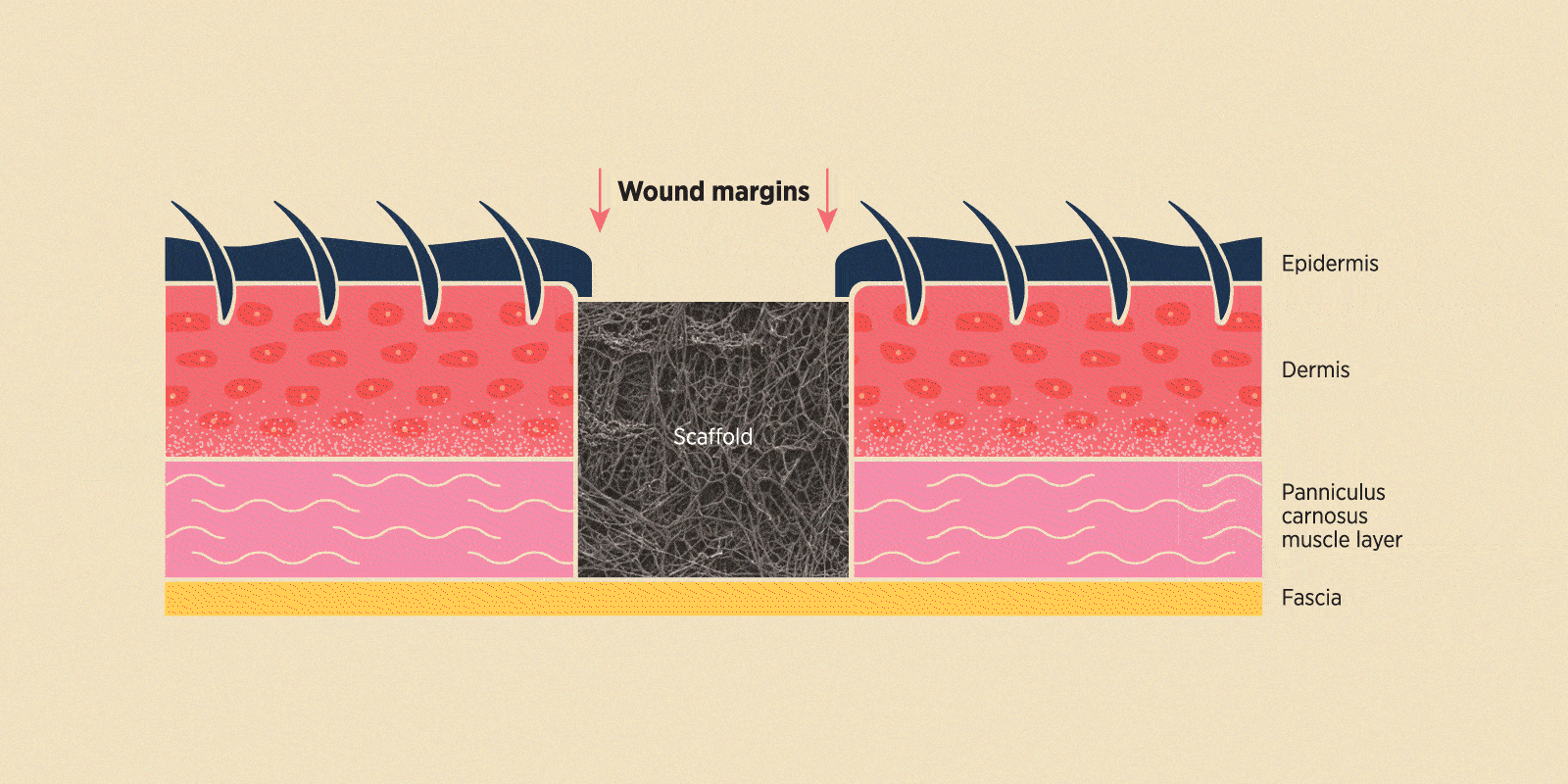
Schematic of a tissue section showing how scaffolds can fill a wound region and act as an artificial dermal matrix. In doing so, they encourage wound repair by providing structural support while functioning as bioactive factors and therapeutic reservoirs.
In their study, Chin and colleagues from the Skin Research Institute of Singapore (SRIS), Nanyang Technological University and University of Auckland explored a method called wet electrospinning to generate dermal scaffolds. The team tested two biocompatible base materials: poly(ℰ-caprolactone), or PCL, alone or as a mixture of PCL and collagen. “[This method] creates a fluffy matrix with a cotton-ball texture,” commented Chin.
They tested their scaffolds in a rat model of wound healing, looking for migration of epidermal keratinocytes and formation of new extracellular matrix within the scaffolds as positive markers of healing. Results showed a significant amount of new extracellular matrix was deposited in the PCL-only scaffolds, forming a foundation for re-epithelialisation and wound closure. Conversely, PCL/collagen scaffolds triggered sustained inflammation and inhibited healing.
“It’s a bit complicated,” said Chin, adding that the lack of structural stability after the addition of collagen might be setting off an inflammatory response that hindered healing. On the other hand, there were clear signs of healing in just five days with the PCL-only scaffolds, suggesting that applying this material as a dermal substitute might also benefit patients with chronic wounds.
Ongoing work by the team is focused on adapting these scaffolds into localised delivery systems for providing additional chemical cues to encourage wound healing. Such systems are superior to oral medications or gels and creams that typically have short half-lives and suffer from poor patient compliance, said Chin.
The lack of healing observed with PCL/collagen scaffolds served as an interesting extension to develop a wound model more closely akin to chronic wounds in humans. “We’ve been working with companies to validate their therapeutic molecules for chronic wounds using this model,” Chin shared, adding that the team has filed a patent on their technology.
The A*STAR-affiliated researcher contributing to this research are from the A*STAR Skin Research Labs (A*SRL).





