Just as the fluid nature of air carries planes to their destinations, it also sends virus-laden droplets from coughs and sneezes drifting toward others with startling efficiency. This is why when a new airborne virus emerges, public health authorities must find ways to optimally curb the spread of infections from person to person.
Chin Chun Ooi, a Research Scientist at A*STAR’s Institute of High Performance Computing (IHPC), said science-backed public health measures are vital for minimising case numbers, particularly during the early days of the pandemic. However, social distancing and wearing masks are not one-size-fits-all solutions. Instead, their effectiveness depends on many variables in real-world settings.
In collaboration with Singapore’s Ministry of Health, National Centre for Infectious Diseases, and Land Transport Authority, Ooi led a study on new methods for assessing infection risks in various indoor settings.
“Critical questions, such as the minimum viral dose required for infection; the viral load emitted when individuals cough, talk, or exercise; and the impact of both on infection risk; needed to be answered,” said Ooi. To that end, Ooi and his colleagues designed a two-pronged approach to build their risk assessment framework, combining measurements of how droplets move in air with advanced computational simulations.
The researchers used an everyday situation as their test case: a ride home on a double-decker public bus. First, they collected data on how particles circulated on board with the help of a fog machine and a small fleet of particle detectors. They then modified the setup to simulate unique environmental conditions, such as with the windows closed the air conditioning turned on, and the COVID-19-infected individual in different locations.
The study’s results support the importance of mask-wearing: the chances of transmission were greatly reduced for those who masked up. Interestingly, seat choice also influenced the chances of catching COVID-19. Passengers seated behind an infected individual were at higher risk due to the movement of air in the enclosed environment.
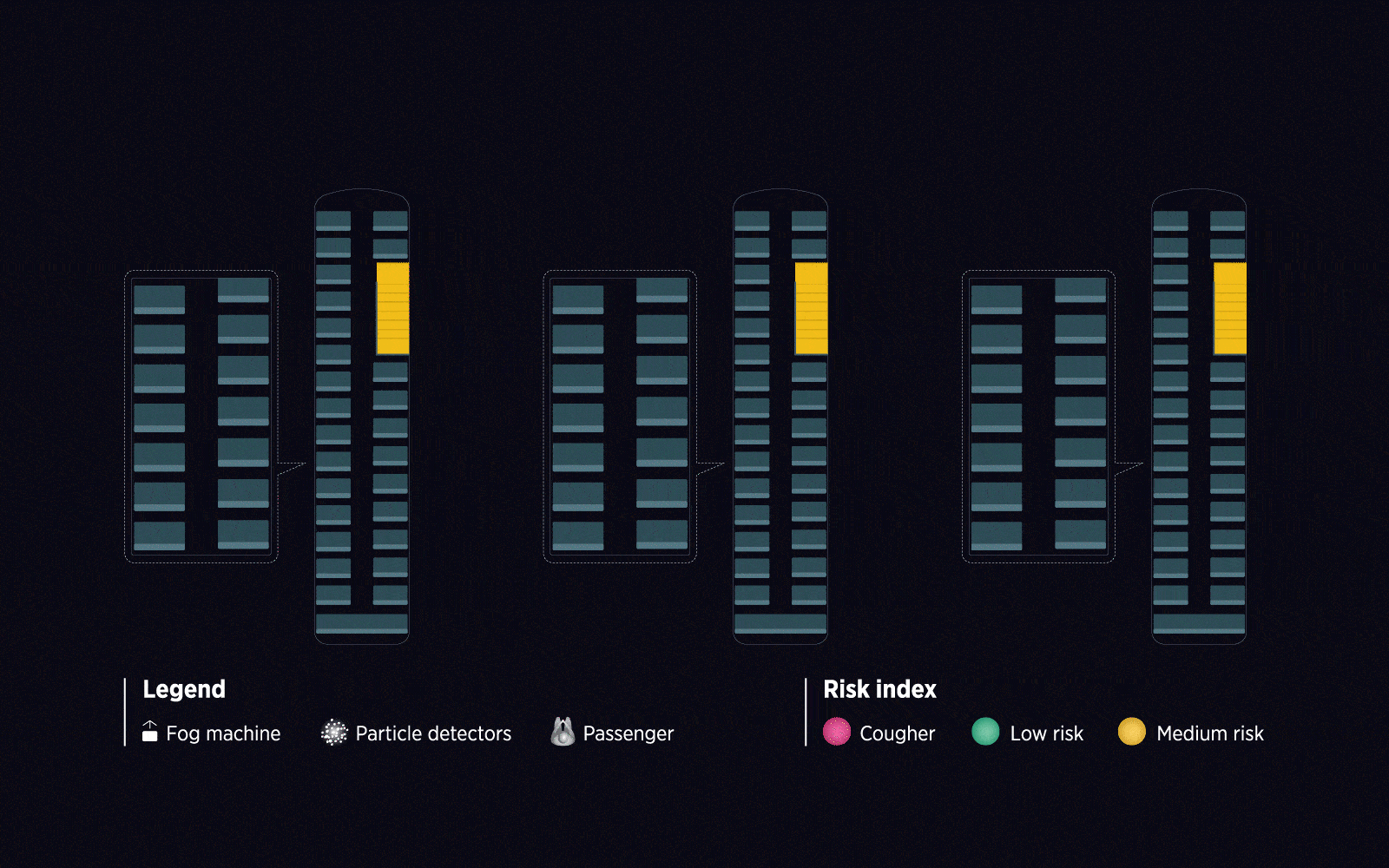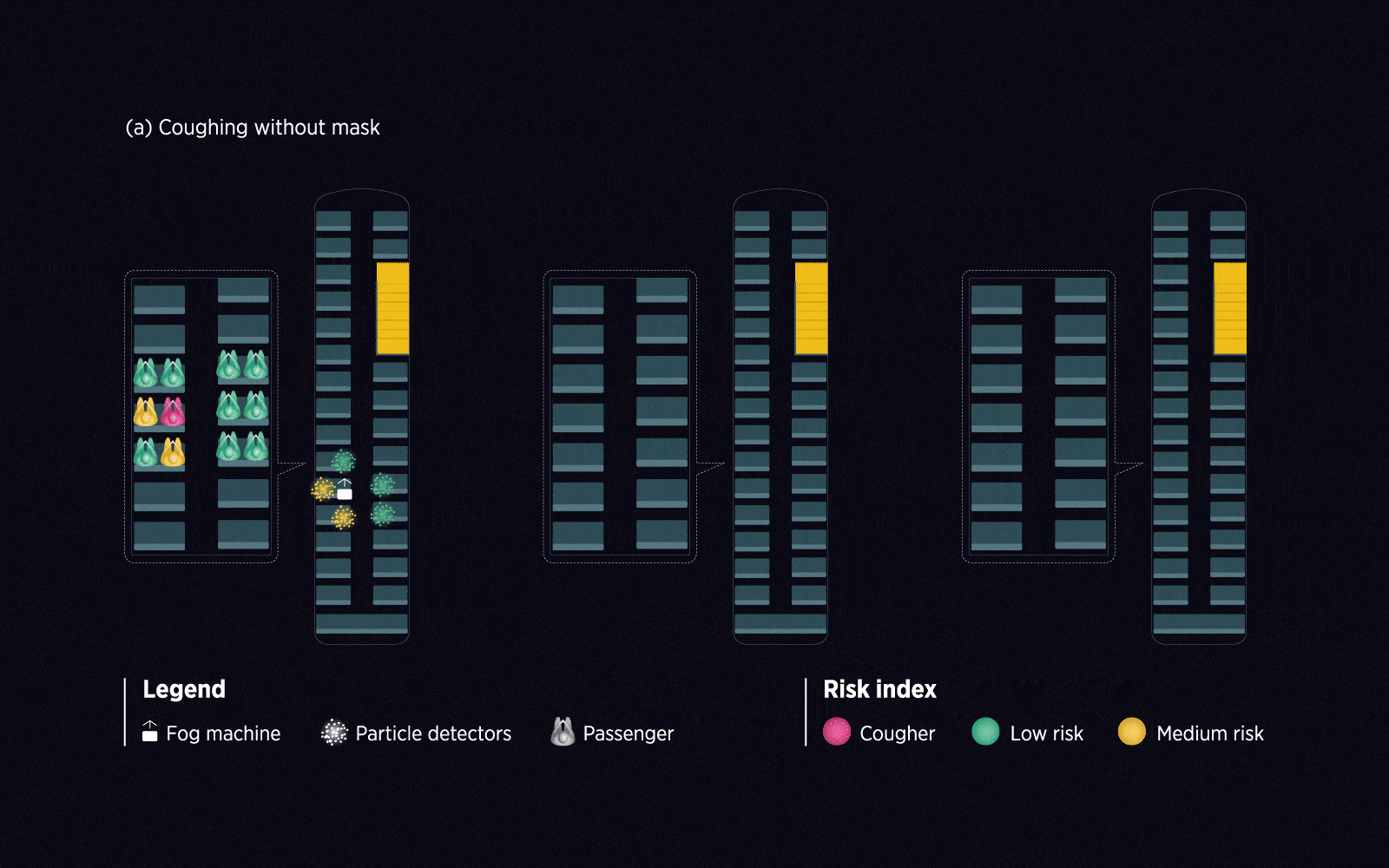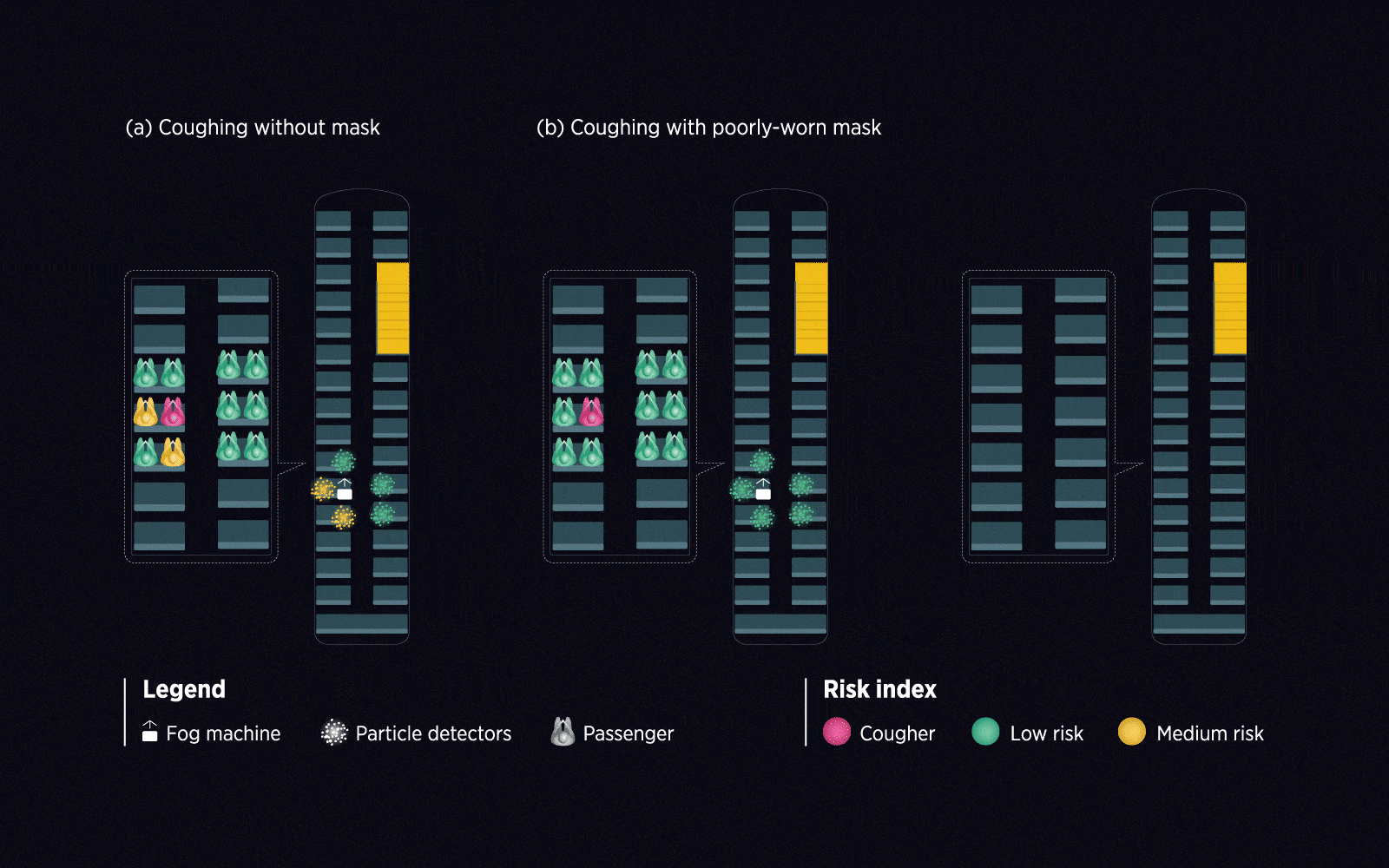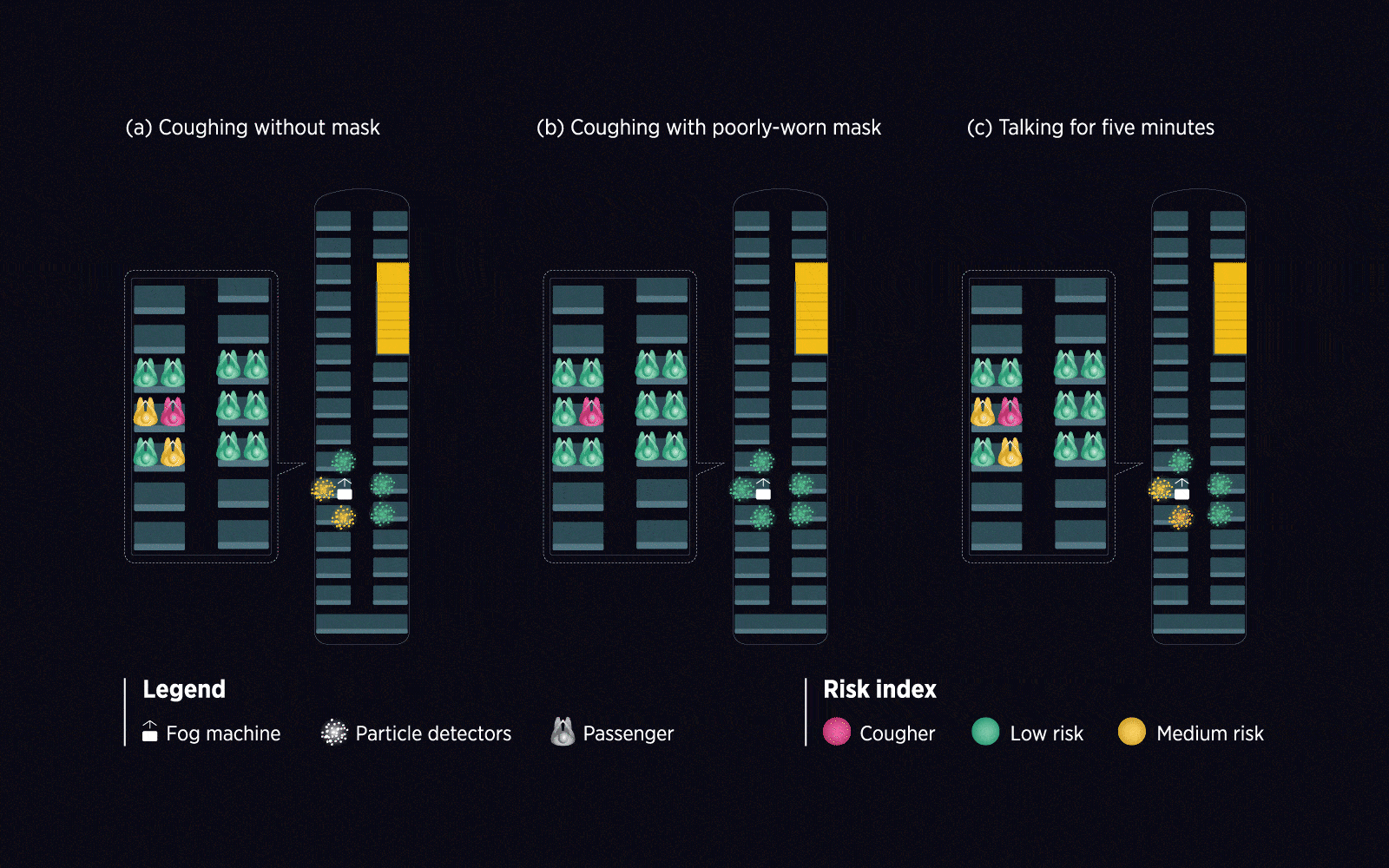
Using live and mathematical simulations, Ooi’s team assessed the relative risk of COVID-19 transmission in a typical double-decker bus from an infected individual in different everyday scenarios.
© A*STAR Research
According to Ooi, these results highlight risk assessment models as vital tools for protecting vulnerable communities against viral threats. “We propose a risk stratification framework that is simple, intuitive, and easily interpretable, facilitating communication and decision-making,” explained Ooi.
The virus has evolved since the study was conducted, sprouting multiple variants of concern with higher transmission rates and prompting the need for updates to the existing risk framework, noted Ooi.
“The viral load thresholds are specific to early variants and will need to be updated with data collected about how more recent variants spread,” said Ooi, adding that these efforts could help to refine and enhance the accuracy of their risk assessment methodology under current circumstances.
The A*STAR-affiliated researchers contributing to this research are from the Institute of High Performance Computing (IHPC) and the Institute of Materials Research and Engineering (IMRE).





