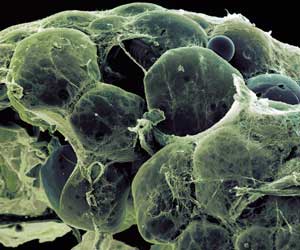
Fat cells that build up around internal organs have higher levels of retinoic acid — a molecule derived from vitamin A — than fat cells in the fat layer beneath the skin.
© Science Photo Library – Steve Gschmeissner/Brand X Pictures/Getty
A molecular mechanism that influences the development of fat cells has been identified by A*STAR researchers. The discovery suggests that an excessive amount of vitamin A could have a role in obesity, and the work could lead to new strategies to ameliorate the risks of fat depositing around internal organs.
Humans have at least two types of fat: subcutaneous fat that sits in a layer beneath the skin, and visceral fat that collects around internal organs. The two fat cell types develop differently and have different properties. Subcutaneous fat is relatively harmless, but visceral fat is considered ‘bad’ or of ‘low quality’, and an excess of it leads to visceral obesity, which is associated with metabolic diseases such as diabetes.
“The contributions of subcutaneous and visceral fat to pathology and physiology are known to be different, but the molecular mechanisms of these differences were unclear,” explains Shigeki Sugii from the A*STAR Singapore Bioimaging Consortium. “By understanding the molecular basis, it is possible to explore therapeutic targeting to improve the quality of visceral fat.”
Sugii and colleagues started from the assumption that the distinct properties of subcutaneous and visceral fat cells arise from inherent differences in the stem cells that they develop from. To look for these differences, they analyzed the gene expression in human fat-derived stem cells from subcutaneous and visceral fat. Their analysis revealed gene expression differences that ultimately led to high levels of retinoic acid in visceral fat cells. Further experiments in cultured fat stem cells showed that retinoic acid inhibits proper development of these cells into mature, functional fat cells. Visceral fat cells are compromised in their proper fat functions, though they can expand in size by gobbling up excessive lipids. The researchers went on to demonstrate that the high levels of retinoic acid were due to its upregulation by a developmental factor called WT1, and that blocking WT1 or retinoic acid signaling reversed the developmental defect in visceral fat stem cells.
“Our findings imply that the developmental origin of visceral fat is different from that of subcutaneous fat, and that this difference results in retinoic-acid-mediated differences in fat cell quality,” says Sugii.

The Fat Metabolism and Stem Cell Group at the A*STAR Singapore Bioimaging Consortium.
© 2016 A*STAR Singapore Bioimaging Consortium
Owing to the relationship between retinoic acid and visceral obesity, Sugii says that his team needs to now look closely at whether excessive intake of vitamin A increases the risk of visceral obesity. He also suggests that their findings could lead to new treatments to prevent visceral obesity and its associated complications, such as metabolic diseases.
“A potential therapeutic approach that targets the retinoic acid signaling pathway would be worth testing for counteracting visceral obesity in animal models,” says Sugii.
The A*STAR-affiliated researchers contributing to this research are from the Singapore Bioimaging Consortium, the Bioinformatics Institute, the Molecular Engineering Lab and the Institute of Medical Biology. For more information about the team’s research, please visit the Fat Metabolism and Stem Cell Group webpage.




