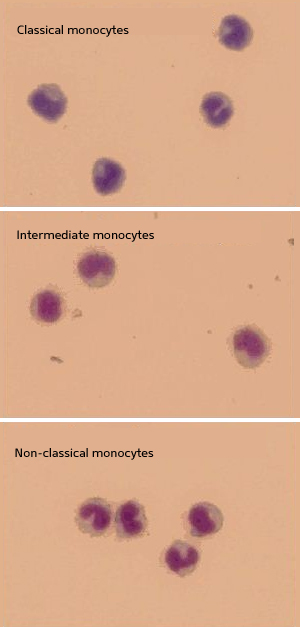
Monocytes are divided into three subtypes according to CD14 and CD16 expression
White blood cells called monocytes can be divided into three subtypes according to their gene expression patterns. Siew Cheng Wong and co-workers at the A*STAR Singapore Immunology Network and Bioinformatics Institute have conducted gene expression profiling on human monocytes and identified several defining features that distinguish one subtype from the other.
Monocytes play a number of important roles in the immune system, including defence against pathogens and maintenance of tissue homeostasis. The traditional classification system used to divide monocytes into two subtypes according to their surface protein expression. The latest classification system, approved by the Nomenclature Committee of the International Union of Immunological Societies, divides monocytes into three subtypes: classical, intermediate and non-classical.
Classical monocytes are monocytes with a high level of CD14 expression. They account for approximately 85% of the total monocyte population. Intermediate monocytes are monocytes with high CD14 and low CD16 expressions. They account for approximately 5% of the total monocyte population. Non-classical monocytes are monocytes with low CD14 and high CD16 expressions. They account for the remaining 10% of the total monocyte population.
Different monocyte subtypes are known to have different gene expression patterns, but the exact details have yet to be elucidated.
Wong and her team purified monocytes from the blood of healthy donors, isolated RNA from the samples and used microarray technology to profile the expression level of each gene. They used a technique called flow cytometry to examine the expression level of each cell surface protein.
The researchers then analyzed the production of small signalling molecules called cytokines and chemokines by each subtype in response to lipopolysaccharide, a cell-wall component found on gram-negative bacteria. They found that at the molecular level, intermediate and non-classical monocytes are very closely related to each other. One way to distinguish between the two monocyte subtypes is to use novel cell surface markers, such as ‘MHC Class II’ molecules.
Another way to distinguish between different monocyte subtypes is by gene markers. Non-classical monocytes, for instance, express high levels of genes involved in cytoskeletal re-arrangements, whereas intermediate monocytes express highest levels of genes involved in T cell interactions. In addition, classical monocytes express the broadest range of receptor genes, and genes involved in tissue repair and immune response.
The findings could have important clinical implications, as the differences in gene expression between the subtypes could aid diagnosis of blood cancers and other haematological disorders. “The proportion of CD16 monocytes increases in many disease conditions,” says Wong. “We therefore plan to analyze monocyte subtypes in different disease conditions. This way, new diagnostic and therapeutic markers can be revealed, and the involvement of monocyte subtypes in specific diseases could be better clarified.”
The A*STAR-affiliated researchers contributing to this research are from the Singapore Immunology Network and Bioinformatics Institute.



